Why Psoriasis Severity Fluctuates Even with Ongoing Treatment

Dr Cheong Wai Kwong
Senior Consultant Dermatologist
MBBS (Singapore), MRCP (UK), FRCP (Edinburgh), FAMS (Dermatology)
Psoriasis can be frustratingly unpredictable. You may be following your treatment plan closely, only to find that your symptoms still flare, settle and then return again without clear warning. For many people, this cycle of improvement and worsening can feel discouraging, especially when it seems like treatments that once worked are no longer as effective.
The reality is that psoriasis is a chronic condition that is influenced by a whole range of internal and external factors. Ongoing treatment cannot always produce results in a steady, progressive manner, as flare-ups could still occur in many scenarios.
Understanding why these changes happen is an important step towards managing the condition more effectively and knowing when your treatment approach may need to be reviewed.
What Do Psoriasis Flare-Ups Look Like?
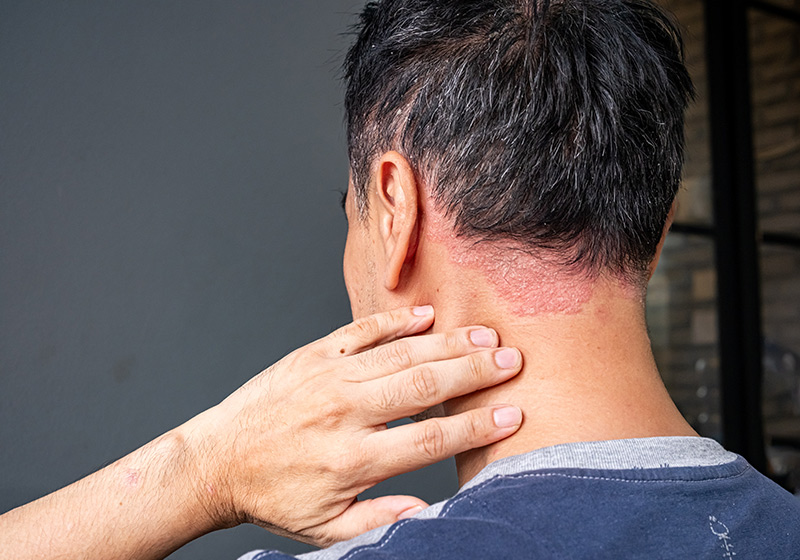
Psoriasis often appears as thick, scaly plaques on areas such as the elbows, knees, scalp and lower back. In other cases, it could appear as smaller patches of irritated, sensitive skin that feel tight or itchy.
During a flare, affected skin may become more inflamed, with increased redness, flaking and discomfort. Some individuals notice that existing plaques become thicker or spread to new areas such as the scalp, elbows, knees or lower back. Others may experience changes in sensation, including burning, stinging or heightened itch that disrupts daily activities.
Common Triggers That Cause Psoriasis Flare-Ups
The root cause of psoriasis is an overactive immune response, which causes skin cells to multiply at an accelerated rate. However, the intensity of this immune activity does not remain constant. Various internal and external factors can stimulate or disrupt your immune system, leading to periods where symptoms become more active or difficult to control.
Flare-ups are typically caused by this immune response. The various triggers could increase inflammation, weaken the skin barrier or place additional stress on your body.
Stress and Emotional Factors
Psychological stress can influence immune signalling in the body, which in turn may worsen inflammation in the skin. Many individuals find that their psoriasis becomes more active during periods of heightened stress, such as demanding work schedules or while undergoing significant life changes.
Infections and Illnesses
In some individuals, a flare may appear suddenly during or shortly after an infection or illness, even if their psoriasis was previously stable.
This happens when certain infections directly trigger psoriasis flare-ups by activating the immune system in a more targeted way. One of the most common causes is streptococcal throat infection (strep throat), which tends to trigger small, drop-like psoriasis breakouts across the body.
Skin Injury
Physical irritation to the skin, even from minor causes like scratches, insect bites or friction, can lead to new psoriasis patches forming in those areas. This is due to the skin barrier being disrupted, which causes the immune system to become overactive again.
Weather and Environmental Changes
Dry or cooler climates can reduce skin hydration and make it more prone to cracking and irritation, which may worsen symptoms. Sudden shifts in weather or excessive sun exposure can also act as stressors on the skin in some individuals.
Medications
Certain medications can interfere with immune regulation or skin turnover, which may trigger or aggravate psoriasis. These include some medications commonly prescribed for blood pressure, mood disorders and inflammation.
Stopping a medication prescription can also result in this effect. Corticosteroids are commonly used to control psoriasis inflammation over long periods of time. Abruptly stopping treatment could cause the skin to react with a sudden surge in inflammation, resulting in a rebound effect.
As these triggers differ between individuals, flare-ups can feel unpredictable unless a patient is well aware of the various possible causes and triggers. This allows them to consult their dermatologist for follow-up treatment in a timely manner.
When Should You Review Your Psoriasis Treatment Plan?
Psoriasis treatments do not produce the same results for everyone. Even with the same diagnosis, patients can experience very different levels of improvement, speed of response and long-term control.
These differences mean that psoriasis management often requires ongoing adjustment. If your treatment is not delivering consistent or adequate control, it may mean that a different or more tailored approach is needed.
You may want to review your treatment plan with your dermatologist if:
- Flare-ups are becoming more frequent
- Plaques are spreading to new areas
- Symptoms are no longer responding as before
- You experience rebound flare-ups after stopping treatment
- Certain areas remain persistently affected
- Itch, pain or discomfort is worsening
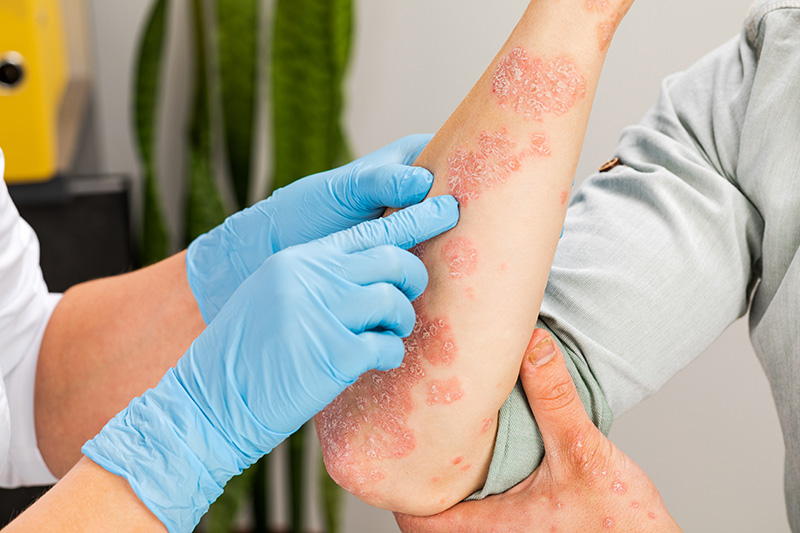
Regaining Long-Term Symptom Control with Dermatologist Support
Psoriasis is a chronic condition that often requires ongoing adjustment from your dermatologist, rather than a fixed approach. Identifying changes and triggers early can allow for more targeted adjustments that help restore better stability. While occasional mild flare-ups may still occur, more frequent, widespread or persistent symptoms may suggest the need for reassessment.
If your psoriasis feels increasingly unpredictable or difficult to control, consulting a dermatologist can help clarify the cause and guide the next steps. Specialist Skin Clinic is a dermatology clinic in Singapore that offers tailored care for skin conditions such as psoriasis, eczema, dandruff and acne. Under the guidance of Dr Cheong Wai Kwong, our senior consultant dermatologist and psoriasis specialist, treatment plans are reviewed on a patient-to-patient basis. Dr Cheong is able to refine various treatment approaches to address flare patterns, improve treatment response and preserve overall skin health.
Contact us today to schedule an assessment and explore treatment options that support more consistent, long-term control.

| Main Line | : (65) 6734 1411 |
| Fax | : (65) 6235 5900 |
| Mon - Fri | : 8:30am - 5:00pm |
| Sat | : 8:00am - 1:00pm |
| Closed on Sundays and Public Holidays | |

