Treating Eczema: Newer Approaches To A Common Problem
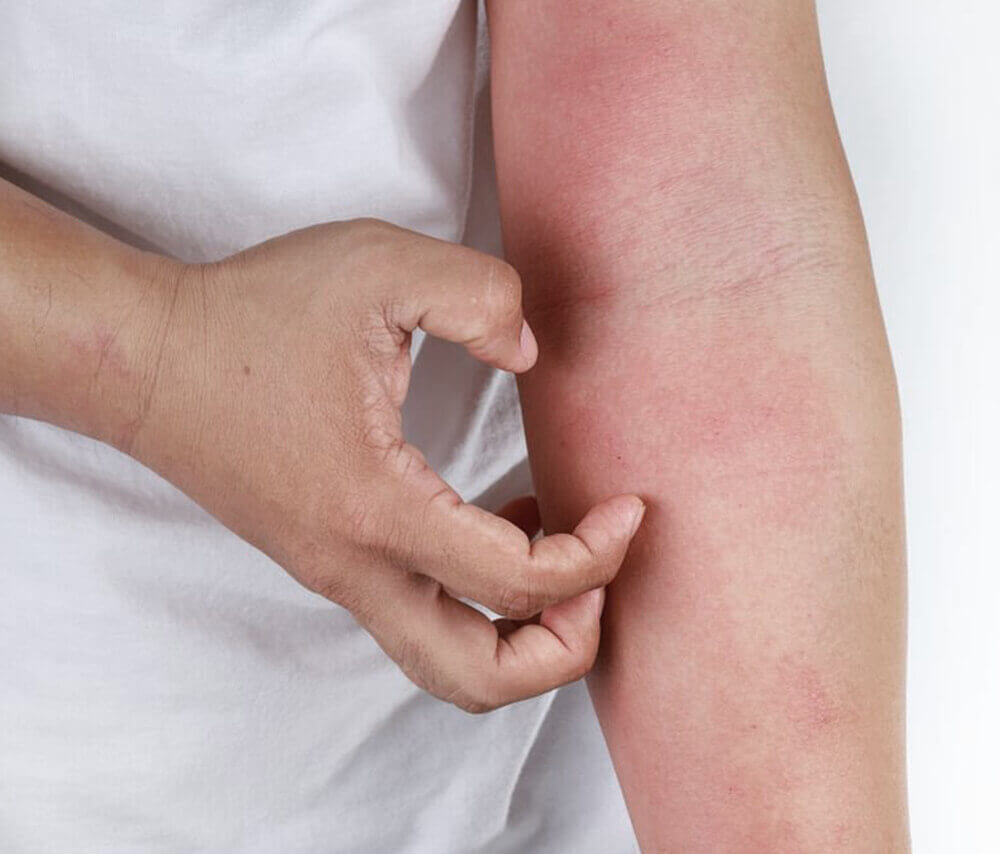
ATOPIC ECZEMA (ALSO KNOWN AS ATOPIC DERMATITIS) IS THE MOST COMMON chronic inflammatory skin disease affecting 20 percent of school going children in Singapore and three percent of adults worldwide. Significant impairment in the quality of life results from poor control as a result of itch and disturbed sleep. Conventional treatments for eczema include frequent generous application of moisturisers, local application of topical steroids (cortisones), wet wrap techniques and oral treatment in resistant disease (cyclosporine or azathioprine). Phototherapy and aggressive treatment of skin infection with antibiotics are also used. With increasing evidence about the underlying skin defects in atopic eczema, exciting new treatments are being explored in the treatment of this otherwise debilitating skin condition.
The recent advance in atopic eczema treatment is the use of an innovative class of barrier therapy. The rationale underlying barrier therapy is that mending the defective epidermal barrier in atopic eczema prevents environmental triggers from penetrating the skin barrier defects. Several of these topical agents purportedly assist in the restoration of the epidermal barrier in eczema through their various ingredients including hyaluronic acid, glycyrrhetinic acid, ceramides and fatty acids.. Although promising in initial studies, the true benefits from their routine long term use in eczema await further scientific trials.
There has been an increased awareness and use of topical immunomodulators (calcineurin inhibitors) in atopic eczema. These topicals do not contain cortisones and thus avoid the concerns from steroid overuse including thinning and weakening of the skin.. The safety and efficacy of these topical calcineurin inhibitors, examples of which are tacrolimus and pimecrolimus, have been demonstrated in many clinical trials. Patients must be counselled about a transient stinging sensation in the first week of use.
The proactive therapy of eczema has also emerged as a possible method to prolong a disease- free period in eczema. This regime consists of twice weekly applications of calcineurin inhibitors (like tacrolimus and pimecrolimus) after eczema has been cleared. This will continue for a period of few months. The rationale for this proactive approach is to try to eliminate remaining inflammation within the normal looking treated skin to reduce flare-ups without risking side effects from use of steroids. In conventional treatment, there is often under-treatment on the part of the patient because of concerns over side effects from steroid use thereby resulting in more frequent flare-up of eczema.
Many other novel therapies which help rebuild the barrier defects, protect against infection and relief of itch in atopic eczema are on the horizon. Patients and physicians can now look forward to these emerging approaches and new therapies for the treatment of atopic eczema.

| Main Line | : (65) 6734 1411 |
| Fax | : (65) 6235 5900 |
| Mon - Fri | : 8:30am - 5:00pm |
| Sat | : 8:00am - 1:00pm |
| Closed on Sundays and Public Holidays | |

